Atopic Dermatitis, also called Eczema
If you or your child has ever had severe eczema (Atopic Dermatitis) flare-up, you are familiar with the inflamed, dry, thickened skin and constant, intense itching and scratching. Fortunately, there are ways to ease symptoms.
An estimated 30 percent of the U.S. population experience symptoms of Atopic Dermatitis, according to the National Institutes of Allergy and Infectious Diseases, but this skin disease is more common among children. Symptoms usually start within the first five years of life, often the first six months. With time and treatment, as children mature, eczema will often go away – but it sometimes continues into adulthood.
Many different factors contribute to eczema, including food and environmental allergens, excessive skin dryness, injury from scratching, and inflammation from bacteria in the skin. Addressing each is essential to controlling the condition.
Eczema and Food Allergens
Although eczema is not necessarily an allergic disease, allergens can play a role. Among infants and toddlers with moderate to severe eczema, it’s often a food allergen.
The most common food allergies in the United States are cow’s milk, egg, wheat, soy, peanuts, tree nuts, and seafood. If you think your child might have food allergies, see a board-certified allergist for an accurate diagnosis before removing any food from your child’s diet.
Environmental Allergens
Common indoor allergens that affect eczema include dust mites and pet dander. To minimize dust mite exposure, encase pillows and mattresses with dust mite covers, wash linens weekly in hot water, vacuum with a HEPA (high-efficiency particulate air) vacuum, and reduce indoor humidity to 40-50 percent, as dust mites need moisture to live.
No measures can effectively reduce pet dander if the animal remains in the home, but it will help to keep pets out of bedrooms and off furniture or rugs where children sleep or play. Pet dander accumulates in house dust, so use HEPA vacuums to keep it down. When all else fails, finding a new home for the pet may be the only option.
Preventing Dry Skin
The skin of children with eczema dries out more rapidly than healthy skin, so it’s important to keep it well-hydrated.
Doctors often recommend the “soak and seal” method – sit the child in a tub of lukewarm water for 15 minutes to let the water soak in, then either shake off excess water or gently pat dry with a towel immediately apply moisturizer in a thick layer. Reapply moisturizer frequently. The National Eczema Association recommends ointment moisturizers rather than lotions or creams.
Topical Corticosteroid Medications
Many children require topical corticosteroid skin ointments or creams to control their eczema fully. These come in a wide range of strengths, so always ask your physician which medications and treatment options are best suited for your child.
Controlling the Itch
Controlling the itch is crucial: The more the child scratches the skin, the more eczema worsens, and symptoms can spiral out of control. Over-the-counter antihistamines may help take the edge off the itch and allow for a better night’s sleep. Some parents find wrapping wet cloths around affected skin eases the itch and stops scratching.
If your child’s eczema remains poorly controlled, consult your board-certified allergist for further treatment options.
Adapted from Allergy & Asthma Today magazine’s “Eczema and Allergies” by John Lee, MD, clinical director of the Food Allergy Program at Boston Children’s Hospital.
Other Resources for Atopic Dermatitis:
Symptoms of Atopic Dermatitis
Atopic Dermatitis, a form of Eczema, is a chronic inflammatory skin disease that causes many different symptoms, which can take many forms and vary from person to person. Several symptoms may be present at the same time.
The most common indicators are:
- dry skin all over the body
- severe itching, especially at night
- skin inflammations that occur repeatedly
- Red patches
- Small, raised bumps, which may leak fluid and crust over when scratched
- Raw, sensitive, swollen, or thick skin from scratching
Symptoms of atopic dermatitis are not constant. They can disappear for a while. However, even if nothing can be seen on the skin surface, inflammation is still present under the skin and will eventually reappear on the outside.
Other symptoms associated with atopic dermatitis include:
- Chronically itchy, scaly skin: itchy skin areas are usually scratched, which makes them even itchier. However, these skin areas are often scratched out of habit, which causes the affected skin to become discolored, thick, and leathery.
- Skin infections: Repeated scratching can cause open sores and cracks. This is an open door for Bacteria and viruses.
- Hand dermatitis: people who clean or disinfect their hands often can develop hand dermatitis.
- Allergic contact dermatitis: it appears after direct contact with a substance or an allergic reaction to it. Many substances can cause such reactions, including soaps, cosmetics, fragrances, jewelry, and plants.
- Asthma and hay fever: Atopic dermatitis is often a precursor to asthma and hay fever. Children who have suffered from atopic dermatitis symptoms in their early years are 50% more likely to develop asthma and hay fever as teenagers.
- Sleep disturbances: Because of the perpetual itching, many people have trouble falling asleep and sleeping through the night. The sleep disturbances worsen Atopic Dermatitis. This is a vicious cycle.
Atopic Dermatitis symptoms often appear on the following parts of the body:
- face
- neck
- hands
- wrists
- elbows
- knees
- ankles
- feet
The following skin areas are affected depending on age:
- Babies: The face – especially the cheeks. AD may spread to the upper body and limbs.
- Infants: The ankles, wrists, limbs, including fingers and toes.
- Older children and adolescents: Folds of the joints (elbows and knees), also the back of the hands, feet, and fingers.
- Adults: in addition to the areas typical of older children and adolescents, there are also the neck, eyelids, and face.
Sources:
https://www.mayoclinic.org/diseases-conditions/atopic-dermatitis-eczema/symptoms-causes/syc-20353273
What is Eczema from Allergy & Asthma Network
https://drustvoad.si/atopijski-dermatitis/
Treatment for AD
There is no standard therapy for all patients with atopic dermatitis. Each patient must be treated individually. Therefore, there is also not only one possible therapy for atopic dermatitis. The treatment consists of 5 elements:
- Avoidance of triggers
- Skincare
- Treatment of itching
- Treatment of inflammation
- Training and rehabilitation
Avoidance of atopic dermatitis-triggers
First of all, it is essential to know what triggers the atopic dermatitis episode. This can be dust mites, animal hair, detergents or cleaning agents, food, etc. Also, the weather can play a role.
A corresponding test can be made at the dermatologist or in appropriate laboratories. Consistent avoidance of the trigger is the fundament for the treatment of eczema.
Skin Care
Skin requires daily care with moisturizing and refatting ointments or lotions that are natural and free of preservatives. PH-neutral products are preferable for cleansing the skin.
Many conventional bath additives or shower gels rob the skin of its protective barrier. These are, therefore, better avoided. The same applies to liquid soaps and surfactants. Salt as a bath additive can help bind the water in the skin and make it more supple. Especially helpful are refatting shower gels and bath oils.
After showering or bathing, the skin should not be rubbed dry. Just lightly dry or dab it dry. Immediately after showering or bathing, apply the moisturizing care product you have received from your doctor or pharmacist for daily use.
Treatment of itching
Itching is excruciating in atopic dermatitis. The more it is scratched, the more inflammation occurs. This is a vicious cycle. Only consistent trigger avoidance, skincare, and adherence to the doctor’s treatment recommendations will improve the itching.
Keep children’s nails as short as possible to avoid injury. In an emergency, you can also put on gloves for the child.
Wet wrap therapy can also be helpful. After doing a soak-and-seal warm bath and applying the medication, the patient’s eczema-damaged skin is wrapped in a layer of wet cloths, often topped by dry clothes – such as pajamas, sweatshirts, or tube socks.
Treatment of the inflammation
The inflammations are generally treated with skin ointments and systemic medications.
Treatment of the skin
Mild to moderate inflammations are usually treated with anti-inflammatory cortisone ointments. Cortisone has an anti-inflammatory effect and is used primarily for acute episodes. Because of its side effects, cortisone should only be used for short periods. In addition, preparations containing cortisone are not suitable for all skin areas (e.g., face, genital area). Therefore, calcineurin inhibitors should rather be used in these areas. These creams also have an anti-inflammatory effect.
Besides cortisone ointments, the following products are also used for the treatment of atopic dermatitis.
Systemic treatment
Severe cases of atopic dermatitis are treated with systemic medications. On the one hand, corticosteroids can be prescribed orally or as injections, and on the other hand, there are so-called biologic treatments, which are used as injection therapy.
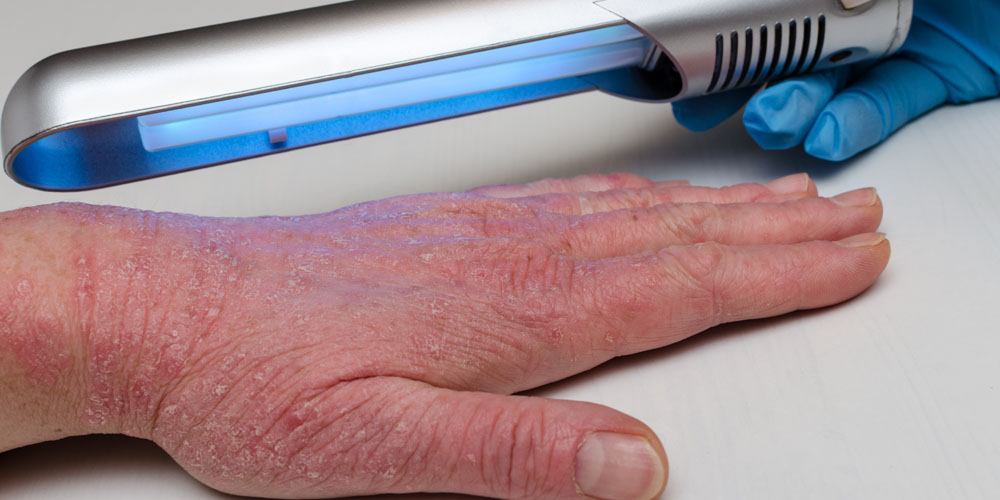
Phototherapy
Phototherapy is the treatment of the skin with electromagnetic rays, mainly in the ultraviolet (UV) range. UVA rays penetrate deeper into the skin and can, therefore also combat deeper-lying inflammatory foci. High-dose UVA radiation therapy can be used for atopic eczema. Low-dose UVA radiation is used in PUVA therapy.
PUVA means that the effect of the UVA rays is intensified with the active drug ingredient Psoralen. Psoralen is administered to the patient by means of capsules in the form of baths or ointments (if only individual areas of the body such as hands or feet are affected). The combination of Psoralen and UVA has proven to be very effective in many skin diseases, as this therapy exerts pronounced inflammation-suppressing effects.
In comparison, UVB therapy only penetrates the more superficial layers of the skin. This form of irradiation is comparable to natural sunlight. Pure UVB therapy is very easy to perform, has few side effects (can also be used on pregnant women, children or patients with a history of tumors), and is similarly effective as PUVA therapy for many skin diseases. In addition to suppressing inflammatory skin processes, all phototherapies also lead to the tanning of the skin.
Training and rehabilitation
In training courses for atopic dermatitis, patients learn how to deal with the disease in everyday life and at work. Information and practical tips for proper skin care, nutrition, dealing with relapses, or relaxation techniques are offered.
Rehabilitation may be considered for severe eczema and a course of the disease with hardly any symptom-free periods. The aim here is to improve the treatment so that it is possible to continue working.
Often eczema and itching lead to sleep problems, which can also put a psychological strain on the patient. Relaxation exercises often help here. If the psychological complaints are pronounced, psychological therapy may also be an option.
Sources
- https://allergyasthmanetwork.org/allergies/food-allergies/
- https://allergyasthmanetwork.org/what-is-eczema/
- https://www.mayoclinic.org/diseases-conditions/atopic-dermatitis-eczema/symptoms-causes/syc-20353273
- https://www.mayoclinic.org/diseases-conditions/atopic-dermatitis-eczema/diagnosis-treatment/drc-20353279
- https://drustvoad.si/atopijski-dermatitis/
- https://www.aad.org/public/diseases/eczema/types/atopic-dermatitis
- https://www.aad.org/public/diseases/eczema/types/atopic-dermatitis/crisaborole
- https://www.aad.org/public/diseases/eczema/childhood/treating/topical-calcineurin-inhibitors
- https://www.aad.org/public/diseases/eczema/childhood/treating/coal-tar